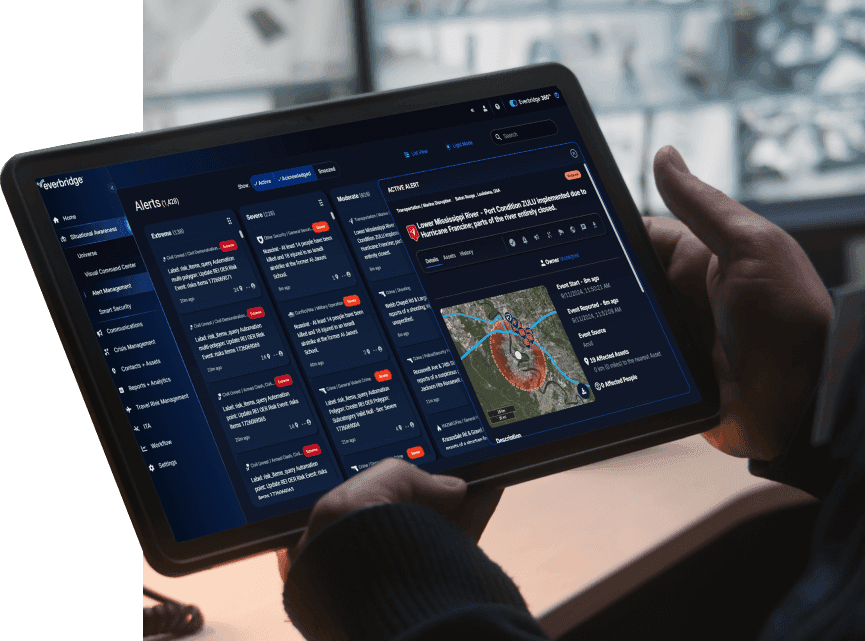
Protect your healthcare or hospital operations with Everbridge
Protect lives, enhance care continuity, and ensure seamless operations with our best-in-class critical event management platform. Everbridge empowers healthcare and hospital providers with a unified platform to detect threats, communicate effectively, and respond rapidly, ensuring patient safety and care continuity even in the most critical moments.

Keep your people safe and your organization running
Hospital and healthcare organizations face unique challenges that require swift, coordinated responses to protect patients, staff, and facilities. From natural disasters and cyberattacks to infectious disease outbreaks, hospital and healthcare organizations must maintain operational resilience while delivering essential care. By harnessing our High Velocity Critical Event Management™, platform, Everbridge 360, organizations can minimize downtime and ensure operational continuity. Powered by Purpose-built AI, Everbridge 360, enables healthcare organizations to deliver uninterrupted services while safeguarding patients and staff.

Know earlier, respond faster, and improve continuously in how you deal with threats
Stay ahead of physical and digital threats like weather events, active assailants, or IT disruptions with our High Velocity Critical Event Management™ platform, Everbridge 360.

1. Know earlier
With advanced business continuity planning and leading risk intelligence, you’ll get real-time insights to detect threats wherever they arise, helping you quickly identify risks to your people and operations.
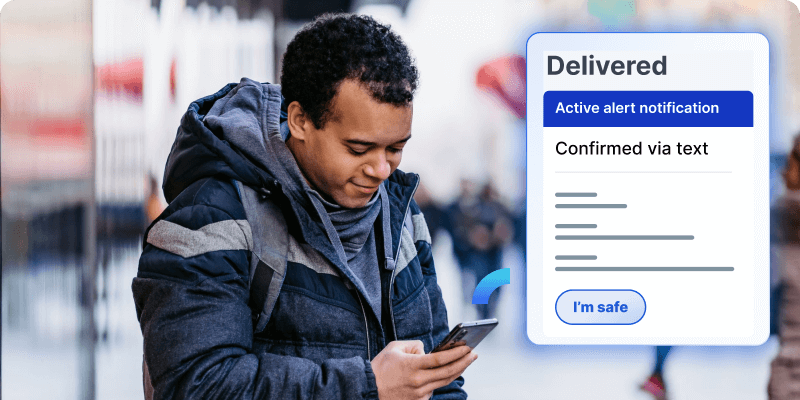
2. Respond faster
When critical events happen, speed matters. Our Alert Management feature enables seamless, “one-click” responses, from emergency communications to clear instructions, keeping your employees safe and your business protected.
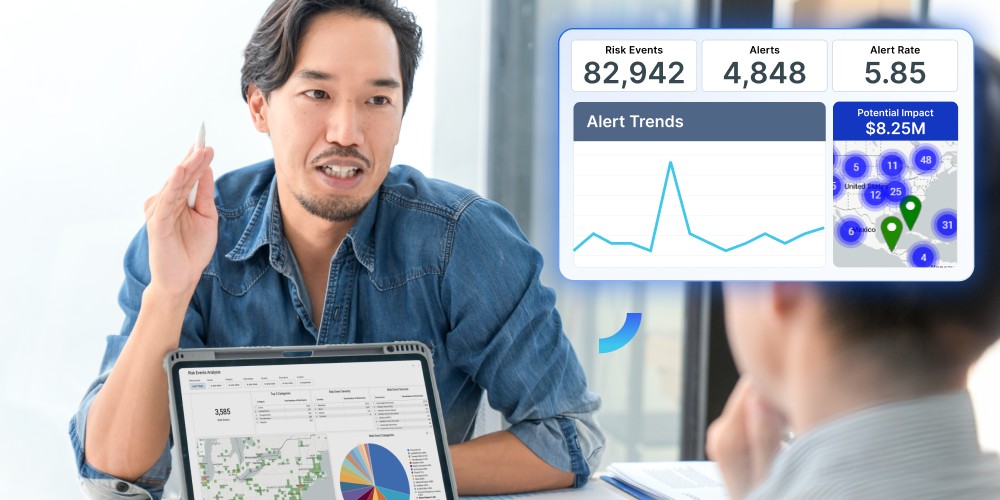
3. Improve continuously
Adapt and improve with our detailed after-action reports, response analytics, and interactive dashboards. Turn data into insights to strengthen your organization’s resilience for the future.
How Everbridge empowers hospital and healthcare organizations
Proactive threat detection
Access real-time risk insights to identify and mitigate potential threats to patients, staff, and facilities before they escalate.
Efficient response workflows
Streamline emergency response efforts with automated workflows to reduce downtime and enhance efficiency for patients.
Seamless communications
Enable two-way communication to coordinate critical responses effectively, ensuring the safety of healthcare teams and delivering clear directives during emergencies.
Enhanced resilience
Leverage advanced risk intelligence and automation to maintain operational continuity, safeguard sensitive data, and meet stringent healthcare compliance standards.

How it works
Everbridge 360 combines advanced risk intelligence, automated communication, and coordination tools. It enables you to identify threats earlier, mobilize the appropriate teams quickly, and recover operations more efficiently. Powered by Purpose-built AI and harnessing real-time data, Everbridge 360 can alert staff during emergencies more efficiently, and minimize downtime in critical systems. Our platform ensures a fast, organized, and effective response, ultimately protecting lives and maintaining care standards during any disruption.
Bringing acute inpatient care home with coordinated, accurate communication
Brigham and Woman’s Hospital is leveraging highly monitored and coordinated communication – enabled by Everbridge CareConverge – between physicians, in-home caregivers and patients, the program is proving beneficial for both the healthcare system and patients.

How your healthcare organization can benefit from using Everbridge
Critical event management
Protect your team and keep your organization secure by staying prepared for any critical situation. With Everbridge 360™, reduce risks, safeguard critical functions, and maintain uninterrupted operations, giving you the confidence to focus on what matters most.
Business continuity
Stay resilient and maintain trust with seamless operations, even in challenging moments. Proactively protect vital data, minimize downtime, and deliver consistent services to your patients, ensuring stability and reliability during disruptions.
Travel risk management
Ensure the safety and well-being of healthcare professionals and lone workers traveling or working remotely with real-time risk alerts and actionable solutions. Keep your team protected and focused, allowing for uninterrupted patient care and continuity.
Digital operations
Deliver exceptional reliability and patient satisfaction by ensuring uninterrupted operations. With proactive solutions that eliminate potential disruptions you can ensure that your systems will run smoothly.

Everbridge named a Leader in The Forrester Wave™: Critical Event Management
Empower resilience with the leading critical event management platform.
Outcome
Healthcare organizations using Everbridge experience improved crisis readiness, faster recovery times, and greater operational continuity. Patients and families benefit from uninterrupted care during emergencies, while staff safety is prioritized. The platform ensures compliance with industry regulations and enhances organizational reputation by mitigating impacts from critical events. Everbridge empowers healthcare providers to deliver care confidently, knowing they are equipped to handle any challenge with precision and trust.
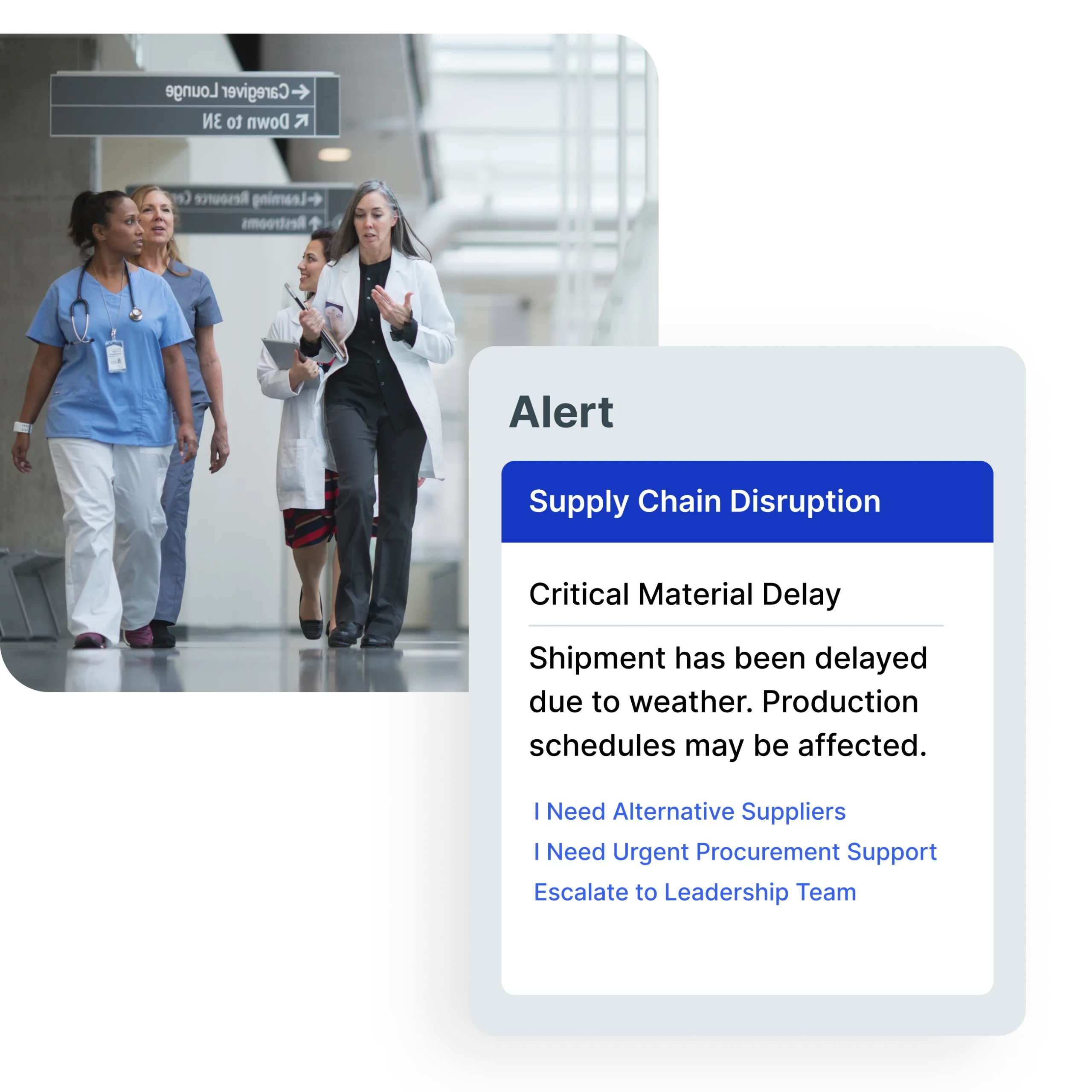
Featured customer stories

Renown Health improves patient care with Everbridge
Renown Health selected Everbridge Mass Notification to help solve
their operational challenges.

Healthcare company uses Everbridge Mass Notification to send critical alerts
Anytime there is a major event—outages, weather situations, this healthcare company uses Everbridge Mass Notification to send critical alerts.

Streamlining stroke notifications and improving patient care
With xMatters, Intermountain Healthcare can streamline notification processes, reduce operational pain of reaching doctors over long distances, and provide patients with the best possible care.

CareConverge clinical case study: Stroke response
The CareConverge solution was deployed at a level I Stroke center in northern Florida with the following goals; time savings, improved in-route patient evaluations and mobile use of telemedicine tools.

Healthcare company plans for another 25 years with Everbridge
Everbridge helped them in front of issues. Their directors spent time traveling between campuses. We needed a mechanism to get notifications to them regardless of where they were.

BC in the Cloud® helps Houston Methodist Hospital triage power outage
Houston Methodist Hospital relies on Everbridge for an uninterrupted stream of reliable data for everything from operating cutting-edge medical devices during lifesaving procedures to scheduling, filing, reporting, and tracking employee hours.
Featured resources

Global Threat Outlook 2025
Download our newly released report “Global Threat Outlook 2025.” This new report will provide essential insights and strategies for navigating the intricate landscape of global threats.

2025 Global Enterprise Resilience Report
Download the report for analysis on industry surveys, insights into the threats resilience leaders are watching, and ways to adopt a more flexible and effective approach to readiness.

Emergency preparedness solution for hospitals & healthcare systems
The Everbridge Emergency Preparedness solution enables healthcare systems to rapidly contact all staff, volunteers, contractors, and other stakeholders with the right information at the right time about an event while meeting the latest CMS regulations.